Herpes and Pregnancy
"All the Important Information"
Herpes and Pregnancy - Overview
Herpes and pregnancy can occur at the same time. In fact 20% to 25% of pregnant women worldwide have genital herpes - some experience periodic herpes lesions and some are asymptomatic (never experienced an outbreak).
Although the mothers-to-be are not at risk, the unborn baby may be in danger.
The degree of risk the baby faces is dependent on three major factors:
- The herpes infection timeline
- Whether antibodies are present in the mother-to-be.
- Whether there has been enough time for antibodies to develop in the baby before the onset of labor.
As a result of a herpes primary infection, the system produces antibodies to the particular type of virus involved.
For example, if a woman contracts genital herpes brought about by the HSV-2 virus, approximately six weeks after the primary outbreak the resultant antibodies in her system will prevent infection of an additional form of HSV-2 herpes on a different part of her body.
The same applies to the oral herpes HSV-1 variety.
What’s more important regarding herpes and pregnancy, after six to nine weeks, the baby will acquire antibodies via the placenta.
Once that has happened, it’s extremely difficult for cross infection to occur while the infant is still in the womb.
It also makes it unlikely that the baby will become infected if the mother happens to be in the viral shedding stage during birth.
Herpes and Pregnancy - The Herpes Infection Timeline
There are three possible scenarios if herpes and pregnancy coincide:
- If the woman had herpes before becoming pregnant, antibodies will be present in her system and she will transfer them to the fetus.
If the mother is in the viral shedding stage during labor, there is less than 1% chance of the baby becoming infected during vaginal birth.
- If primary infection occurred shortly before, or during the first trimester of pregnancy, the unborn baby is at risk.
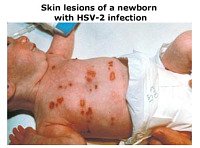 Since it takes approximately 6 weeks for antibodies to develop in the fetus, there is a 3% chance of the infant becoming infected by viral shedding during vaginal birth.
Since it takes approximately 6 weeks for antibodies to develop in the fetus, there is a 3% chance of the infant becoming infected by viral shedding during vaginal birth. In rare cases, transmission could occur via the placenta. In this instance there is a 5% possibility of the baby being born with serious birth defects.
- If primary infection occurred during the second or third trimester of the pregnancy, this situation presents the highest risk of transferring the virus to the baby during vaginal birth.
In this scenario, if the virus is shedding during labor, there is an up to 50% chance of the infant acquiring an often fatal neonatal disease. Therefore a Caesarian section, rather than vaginal birth is essential.
The mother may have contracted herpes years earlier and been asymptomatic.
If this was the case, she would have developed antibodies and the outbreak would therefore carry the same risk as a recurrent outbreak from a long-standing infection.
In the case of a first outbreak during pregnancy, the doctor should call for a “Western blot” blood test to:
- Identify the type of virus.
- Tell whether the outbreak was a non-primary first occurrence, or a primary outbreak.
Herpes and Pregnancy - Treatment During Gestation
The American College of Obstetricians and Gynecologists (ACOG) recommend daily suppressive antiviral therapy to be given to herpes positive women from the 36th week of pregnancy.
This limits HSV recurrence and shedding during childbirth, thereby reducing the need for caesarean section.
Since the drug ‘acyclovir’ was subjected to a clinical study of 1000 pregnant women in which there were no increases in birth defects, it remains the drug of choice during pregnancy.
For women infected during the second or third trimester, daily suppressive treatment with antiviral herpes medicine as described above, should be considered.
For others, this antiviral therapy is recommended during the final 10 days prior to delivery.
This will all but eliminate the chances of viral shedding while giving birth.
Herpes and Pregnancy - Vaginal Delivery or Cesarean Section?
- Vaginal birth presents the greatest risk of cross transmission between mother and child.
If lesions are detected on either the cervix, inside walls of the vagina, urethra or on the vulva prior to delivery, a Cesarean section would be necessary.
- If a woman has oral herpes lesions, they should be covered with an occlusive dressing before vaginal delivery.
- In other cases there is less than a 1% chance of the baby suffering from neonatal disease, therefore a vaginal delivery would be the logical option for most women.
Herpes and Pregnancy - Precautions During Pregnancy
- Even if both partners appear to be herpes negative, they must consider the following:
Since 80% of herpes positive victims have never had a primary outbreak, both parties must undergo a herpes blood test as a sensible precaution.
If either partner is infected, they must take antiviral medication throughout the pregnancy.
- Use a latex condom during vaginal, anal or oral sex to reduce the chances of transmission.
- Skip all sexual contact if either partner has a herpes outbreak or experiences prodromal symptoms (tingling, itching or
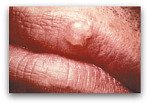 pain in the area of an impending outbreak) during the gestation period.
pain in the area of an impending outbreak) during the gestation period. - Avoid mutual skin contact if either partner develops a cold sore.
- Abstain from sex altogether during the third trimester of pregnancy.
Many sufferers engage in a relentless
Internet hunt for effective remedies, and
this is where interactive websites and
forums, such as our own Pay It Forward
section, play an important part.
----Sidebar----
Herpes and Pregnancy - Post Natal Precautions Q&A
- Q) - How long is my baby at risk from viral shedding?
- A) - It takes about six months for baby’s immune system to fully develop. Daily suppressive antiviral therapy for both parents would be a sensible precaution during this time.
- Q) -
 Can I breastfeed if I have herpes?
Can I breastfeed if I have herpes? - A) - Provided there are no signs of infection to the breast area or to your hands, there is no particular risk involved.
- Q) - Can I kiss my baby?
- A) - Yes, however, if you have facial prodromal symptoms or an active cold sore, wear a disposable surgical mask while handling the baby.
- Q) - What if I have an outbreak?
- A) - Take extra care as detailed above. Once the lesion is fully developed, apply a single dose of Dynamiclear
to the lesions and wash your hands thoroughly with antibacterial soap before handling the baby.
- Q) - How can I tell if my baby becomes infected?
- A) - See your pediatrician at the first sign of a blister or suspicious rash on any part of the infant’s head or body.
Need Help? e-mail us at: remedybusters@gmail.com or click here.
Was This Article Helpful?
If so, a small donation (even $1) would help underwrite the cost of maintaining this website, and allow us to provide even more free home remedy content.
To make a donation, use the button below and fill in an amount. Thanks!
PayPal - The safer, easier way to donate!
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~References
- USDA Agency for Healthcare Research and Quality: Management of herpes in pregnancy
- MedScape: Genital Herpes in Pregnancy
- Herpes.com: Herpes During Pregnancy
Need to speak with someone right away?
Call:
American Social Health Association Hotline: 919-361-8400 (9 a.m. to 7 p.m. Eastern Time, Monday through Friday). Or go directly to the ASHA website.
Back to Home Remedy Site home page, from Herpes and Pregnancy



